Rethinking OCD: New Study Challenges the ‘Serotonin Deficiency’ Theory
For decades, the prevailing medical consensus suggested that Obsessive-Compulsive Disorder (OCD) was primarily the result of a chemical imbalance—specifically, a lack of serotonin in the brain. However, new research published in Nature Communications is shifting this paradigm, revealing that the condition may be linked to how the brain processes serotonin rather than a simple deficiency of the neurotransmitter.

The study suggests that the biological root of OCD lies in the sensitivity and functioning of serotonin receptors, particularly within the prefrontal cortex. This area of the brain is critical for complex cognitive behavior and decision-making, and the findings indicate that the way these receptors interact with serotonin is what drives the symptoms of the disorder.
This discovery provides a crucial explanation for why Selective Serotonin Reuptake Inhibitors (SSRIs), the standard pharmacological treatment for OCD, do not work for every patient. While SSRIs increase the availability of serotonin in the synaptic cleft, they do not address the underlying receptor dysfunction identified in the study. Understanding these cellular mechanisms is a vital step toward developing more personalized and effective mental health interventions.
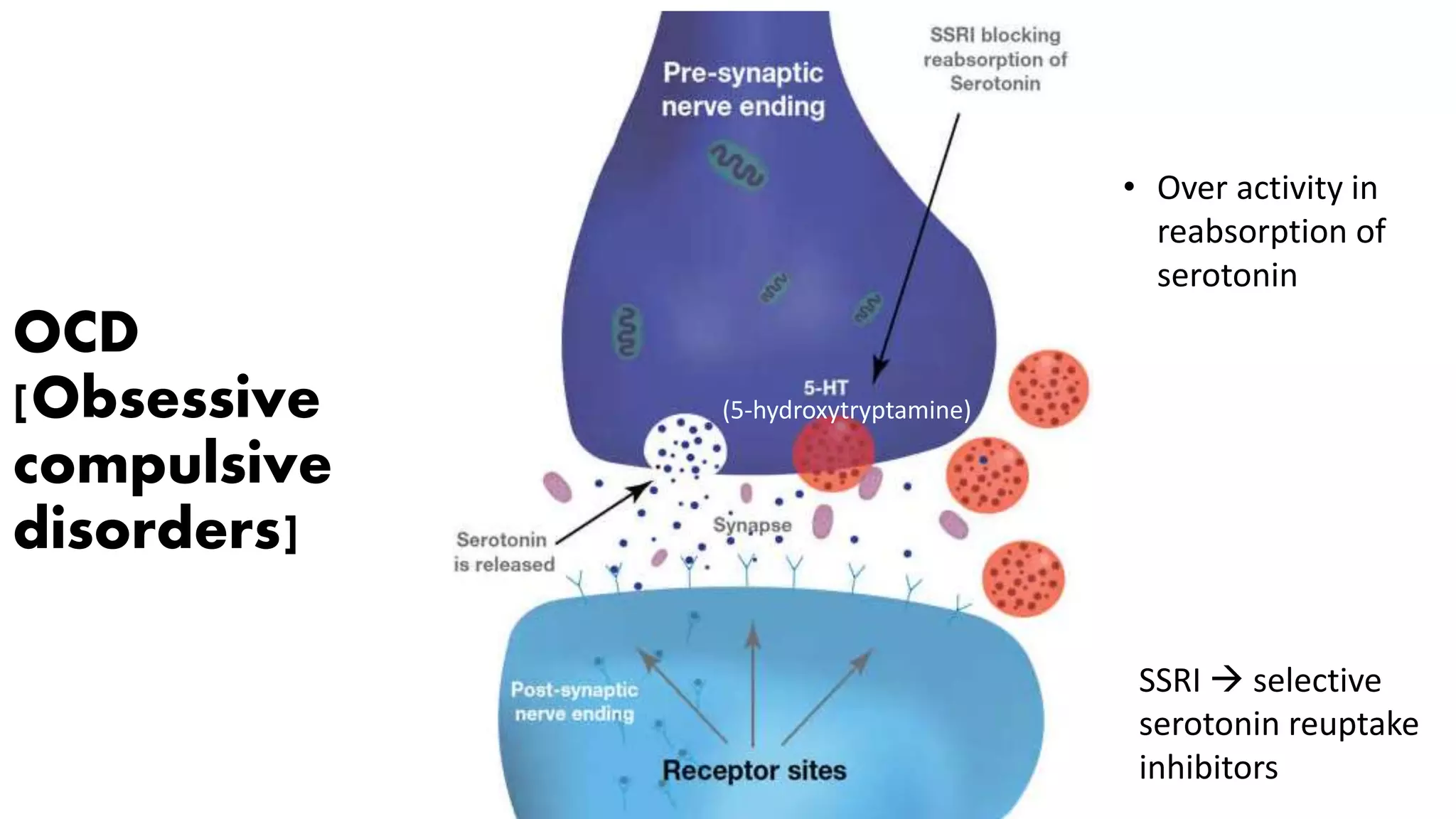
According to the research, the issue is not that the brain lacks serotonin, but rather that the 5-HT2A receptors are not functioning optimally. This distinction is significant for public health, as it moves the conversation away from a generic “chemical imbalance” and toward a more nuanced understanding of neural circuitry and receptor sensitivity.
The findings could guide future treatment strategies, potentially leading to the development of medications that target specific receptors more precisely than current broad-spectrum antidepressants. By focusing on the actual mechanism of receptor dysfunction, clinicians may eventually be able to offer more targeted relief to those who have remained resistant to traditional therapies.
The update underscores the ongoing challenges in treating OCD and highlights the importance of continued research into the brain’s molecular architecture to improve patient outcomes globally.

