Recent medical research has highlighted a critical link between obesity and an increased risk of developing several of the most dangerous types of cancer. According to a study published in JAMA Oncology, which analyzed health data from Germany, Sweden, and the United Kingdom, obesity and being overweight may be associated with a wider range of cancers than previously estimated.
The Scale of the Risk
The findings underscore a significant public health challenge. In the United Kingdom, data indicates that obesity is the second leading risk factor for cancer, trailing only smoking. Health statistics show that approximately 18,000 preventable cancer cases in Britain are linked to obesity. This is particularly concerning given current population trends; in England, roughly 28% of adults are classified as obese (BMI over 30), even as another 36% are considered overweight (BMI over 25).
How Obesity Triggers Cancer
Medical research explains that excessive body fat does more than just add weight; it alters the body’s internal chemistry. Obesity can lead to chronic inflammation and hormonal imbalances, both of which can stimulate the growth of malignant cells. For instance, the World Health Organization and the American Cancer Society have identified at least 13 types of cancer linked to obesity, including:
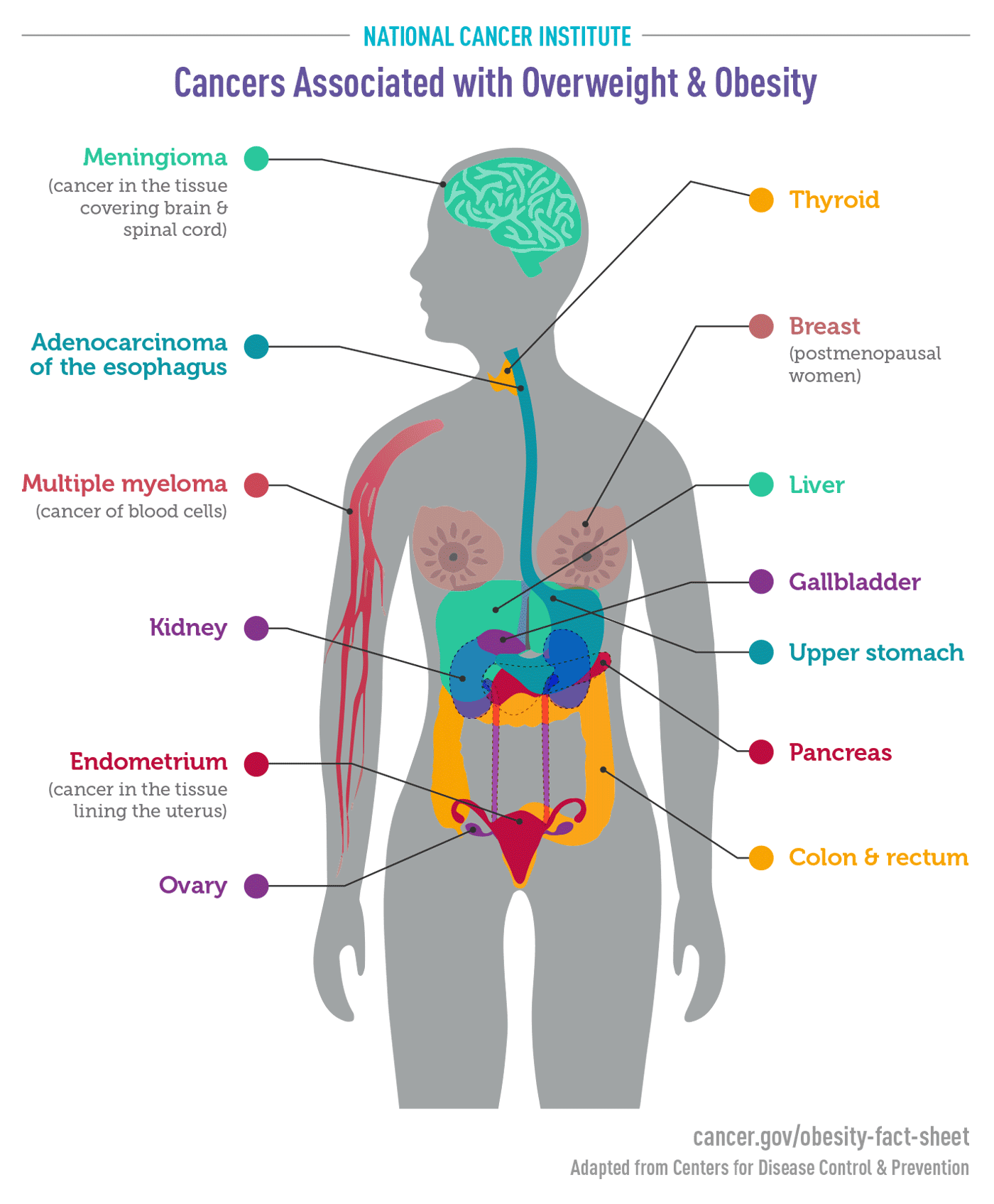
- Postmenopausal Breast Cancer: Increased fat leads to higher estrogen production.
- Colorectal Cancer: Linked to chronic inflammation and slower intestinal motility.
- Liver Cancer: Obesity can lead to liver cirrhosis, which may then progress to cancer.
- Pancreatic Cancer: Often driven by insulin resistance caused by obesity.
- Endometrial Cancer: Fat accumulation increases estrogen levels.
- Kidney Cancer: Associated with hormonal changes and increased blood pressure.
- Stomach and Esophageal Cancers: Linked to abdominal pressure and acid reflux.
New Frameworks for Prevention
To better understand and measure these risks, German researchers have proposed a new framework called “PLUS.” This approach suggests that measuring risk should not rely on a single point in time but should instead consider a person’s weight across their entire lifespan, their waist circumference, and any weight loss that occurred prior to a diagnosis. This comprehensive measurement could help clinicians more accurately identify those at highest risk.
The Path to Prevention
The consensus among researchers is clear: weight management is one of the most effective tools for cancer prevention. Even modest changes can have a significant impact; studies show that losing just 5% to 10% of total body weight can improve vital health markers and reduce systemic inflammation. Research indicates that obesity surgeries may similarly help reduce the long-term risk of cancer.
These findings emphasize that prioritizing weight loss and maintaining a healthy BMI are not just matters of fitness, but essential strategies for reducing the risk of life-threatening malignancies.

