You, and ready
Thyroid cancer diagnoses are rising faster than any other cancer in some parts of the world, prompting concern among medical experts. Understanding the reasons behind this trend is crucial for both patients and public health officials.
In the United States, the incidence of thyroid cancer has increased at a rate exceeding all other cancers. But what’s driving this mysterious “epidemic”?
The thyroid, located at the base of the neck below the Adam’s apple, is responsible for producing hormones that regulate heart rate, blood pressure, body temperature, and weight. Thyroid cancer develops when cells within the thyroid begin to grow and divide uncontrollably, forming a tumor. These abnormal cells can invade surrounding tissues and potentially spread to other parts of the body.
While most cases of thyroid cancer are curable, healthcare professionals are increasingly worried about the speed of its rising incidence. Data from the Surveillance, Epidemiology, and End Results (SEER) Cancer Statistics program in the U.S. shows that thyroid cancer rates more than tripled between 1980 and 2016: increasing from 2.39 cases per 100,000 people to 7.54 for men, and from 6.15 to 21.28 for women.
“Thyroid cancer is one of the few cancers that has continued to increase in incidence over time, even with medical advancements,” said Sanziana Roman, an endocrine surgeon at the University of California, San Francisco (UCSF).
What’s behind the increase in cases? Initially, experts puzzled over the trend, but a key factor emerged: improvements in diagnostic technology.
In the 1980s, doctors began using thyroid ultrasound, a technique that uses sound waves to create images of the thyroid gland. This allowed them to detect very small thyroid cancers that previously would have gone unnoticed.
By the 1990s, doctors also started performing fine needle aspiration biopsies, a procedure where cells are collected from suspicious lumps to determine if they are cancerous.
“In the past, doctors would feel the thyroid for nodules,” explained Cari Kitahara, an epidemiologist at the National Cancer Institute in Maryland.
“But with the advent of technologies like ultrasound, doctors are able to detect smaller nodules and then perform biopsies. This has led to the diagnosis of more small papillary thyroid cancers that would not have been detectable by palpation alone.”
Further evidence supports the theory of “overdiagnosis.” While thyroid cancer incidence has risen rapidly, mortality rates have remained stable. Additionally, a nationwide thyroid cancer screening program in South Korea led to a surge in cases; when the program was scaled back, the number of diagnoses decreased.
“These patterns are consistent with overdiagnosis, meaning that the detected disease may never have caused symptoms or death if it hadn’t been found,” Kitahara said.
Photo Credit: Getty Images / BBC News
It’s now known that small papillary thyroid cancers typically grow slowly and respond well to treatment. They are rarely fatal and have a high chance of being cured. However, during a period of overdiagnosis, many people underwent unnecessary medical interventions, including complete thyroid removal and subsequent radioactive iodine treatment to eliminate any remaining cells. Surgery can sometimes lead to vocal cord paralysis, and radioactive iodine treatment can increase the risk of secondary cancers.
Clinical practice in the U.S. has since adjusted. Radioactive iodine is now only used to treat aggressive cancers, and dosages are minimized to reduce side effects. Doctors are also increasingly opting for partial thyroid removal or a “watchful waiting” approach instead of complete removal.
As a result, the latest statistics from the SEER program show that the number of thyroid cancer cases in the U.S. has stabilized. For example, there were 13.9 new cases per 100,000 people on average in 2010, compared to 14.1 in 2022 (the most recent year for which data is available).
However, some scientists in recent years believe that “overdiagnosis” alone doesn’t fully explain the increase in all cases.
In one study, Riccardo Vigneri, honorary professor of endocrinology at the University of Catania in Italy, pointed out that if overdiagnosis were the only reason, case numbers should have increased more in high-income countries with more sophisticated diagnostic techniques. But this isn’t the case; thyroid cancer incidence is also rising in middle-income countries.
“The incidence of thyroid cancer is rising even in areas without robust screening programs,” Roman said.
“And diagnoses of larger, more advanced tumors are becoming more frequent. This suggests we are facing a dual effect of detection bias and a real increase in disease incidence.”
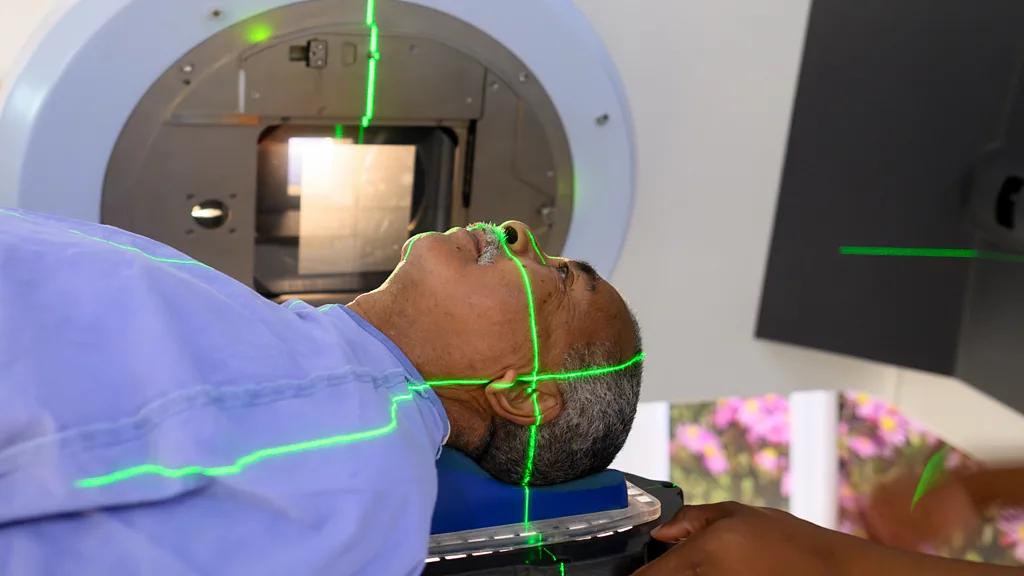
Photo Credit: Getty Images / BBC News
Importantly, as thyroid cancer is diagnosed at earlier stages, treatment outcomes have improved, and theoretically, death rates should decline. However, Vigneri noted that mortality rates have remained at approximately 0.5 deaths per 100,000 people, and have even risen in some countries.
For example, a study analyzing over 69,000 thyroid cancer patients diagnosed in California between 2000 and 2017 found that both the number of diagnoses and the mortality rate increased during that period, indicating that other factors are at play beyond more refined diagnostic techniques.
In 2017, Kitahara and her team also reviewed medical records of more than 77,000 thyroid cancer patients from 1974 to 2013. The results showed that while the increase in cases primarily came from small papillary tumors limited to the thyroid, papillary cancer that had spread to other parts of the body also increased. Although thyroid cancer deaths are rare, the study also showed that mortality rates were increasing by 1.1% per year.
“This suggests that other factors may be driving the increase in these more aggressive tumors,” Kitahara said.
One major suspect is obesity. Obesity rates have risen significantly in the U.S. and other developed countries since the 1980s. Cohort studies (which track healthy populations over time) show a link between excess weight and thyroid cancer risk. People with a higher body mass index (BMI) are more than 50% more likely to develop thyroid cancer in their lifetime compared to those with a healthy weight.
BMI is also associated with characteristics of more aggressive tumors, such as larger tumor size at diagnosis or mutations that make cancer more likely to spread.
“In our studies, we’ve also seen a correlation between BMI and the risk of death from thyroid cancer,” Kitahara said. “This is fairly strong evidence that it’s not just detection bias. It’s not that people with higher BMIs are more likely to get their thyroids checked, it’s that higher BMI itself may be associated with the development of thyroid cancer.”
The mechanisms by which obesity leads to thyroid cancer are still unclear. However, obesity is known to increase the risk of thyroid dysfunction. For example, people with higher BMIs often have elevated levels of thyroid-stimulating hormone (TSH), a hormone secreted by the pituitary gland that regulates thyroid function.
“We don’t fully understand the underlying mechanisms yet, and it’s still an understudied area, but it likely involves multiple factors,” Kitahara said.
“Obesity has many physiological effects, including inflammation, insulin resistance, and changes in thyroid function, all of which could play a role in the development of thyroid cancer.”

Photo Credit: Getty Images / BBC News
Other scientists suspect that “endocrine-disrupting chemicals” (EDCs) found in common household products and pesticides may be a contributing factor. These chemicals mimic, block, or interfere with the body’s hormones. Examples include perfluorooctanoic acid (PFOA) and perfluorooctanesulfonic acid (PFOS), which are found in a variety of items, from cookware and food packaging to personal care products, carpets, and fire-fighting foam. However, the evidence linking these chemicals to thyroid cancer remains inconsistent.
Other research points to trace elements as potentially playing a role. Trace elements are chemicals that the body only needs in very small amounts, but are essential for thyroid function.
“We’ve seen particularly high rates of thyroid cancer in island nations,” Kitahara said.
“Some hypotheses suggest this is related to trace elements associated with volcanic eruptions. For example, chemicals like zinc, cadmium, and vanadium have been detected in these environments alongside high incidence rates, but well-designed epidemiological studies to support a direct causal relationship are still lacking.”
However, Kitahara believes another possible explanation comes from radiation exposure from medical diagnostic scans. Since the 1980s, the number of CT and X-ray examinations in the U.S. and other countries has increased significantly, including CT scans performed on children. These scans expose the thyroid to a relatively high dose of radiation.
Based on the relationship between radiation and thyroid cancer revealed by other studies (such as those of Japanese atomic bomb survivors), we can estimate the impact of this type of medical radiation. For example, a recent study estimated that approximately 3,500 thyroid cancers in the U.S. each year can be directly attributed to the use of CT scans.
“Young people’s thyroids are more susceptible to radiation exposure,” Kitahara said. “Therefore, the increase in CT scan usage may partially explain the increase in thyroid cancer cases in the U.S. and elsewhere.”
It’s also possible that multiple factors are working together.
“We are likely observing a multifactorial phenomenon involving environmental, metabolic, dietary, and hormonal influences, and potentially interacting with underlying genetic susceptibility,” Roman said.
This article was republished with permission from BBC News Chinese, original article available here.
Read More
[Join Key Review Network Membership] Get exciting good articles delivered to your inbox every day, and enjoy exclusive weekly newsletters, current affairs selections, and art and culture reports. Click here to join for free!
Editor: Zhu Jiayi
Review Editor: Ong Shihang
