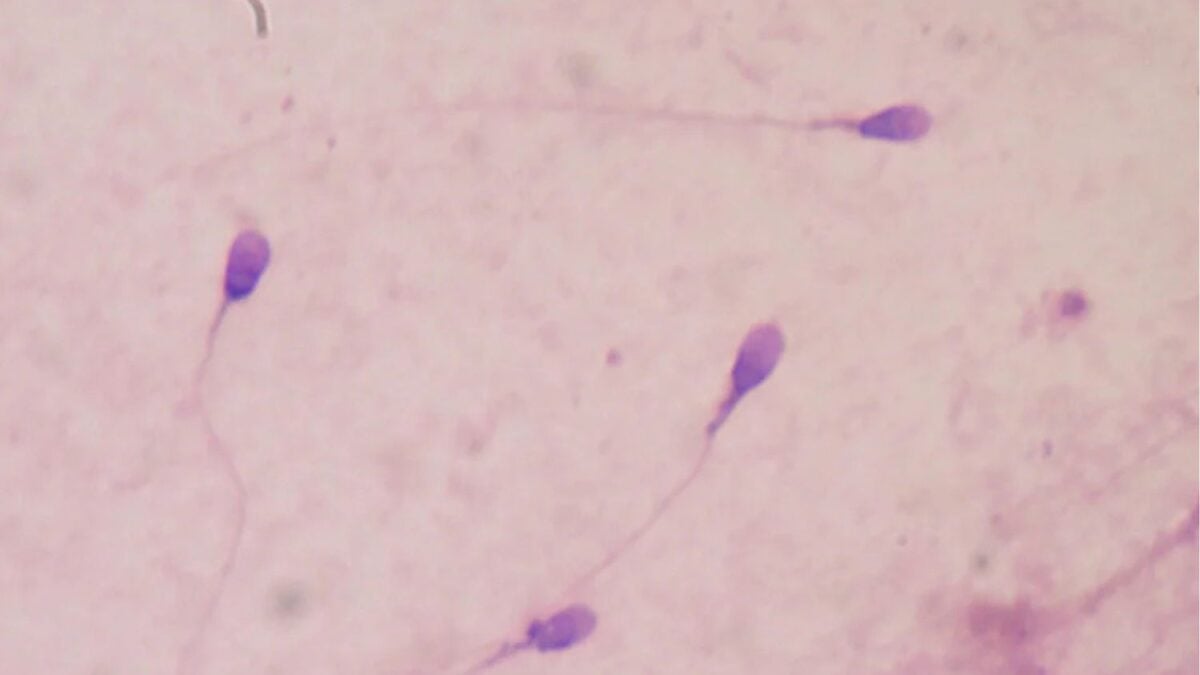
The company Paterna Biosciences, based in Utah, says it has successfully grown functional human sperm in a laboratory and used them to create embryos that appear visibly healthy. The technique could one day help men with certain types of infertility father biological children. The findings have not yet been published in a peer-reviewed journal or independently verified. WIRED was the first to report on this advancement. According to the company, the process involves isolating sperm-producing stem cells from testicular tissue and stimulating their maturation into fully developed sperm in a lab dish. Scientists have spent nearly a century attempting to produce sperm outside the body, a method known as in vitro spermatogenesis. A Japanese team was the first to generate viable mouse sperm in the lab in 2011, but creating human sperm has proven far more challenging. Another biotech firm, Kallistem in France, claimed to have achieved in vitro spermatogenesis in 2015, though outside researchers questioned whether the sperm were fully developed, and the company did not demonstrate they could fertilize eggs. The maturation of sperm-producing stem cells in the body takes just over two months and involves several stages. After production in the testicular tubules, the stem cells undergo meiosis, dividing to create cells with 23 chromosomes. At this stage, sperm develop the tail and head necessary for movement. They then travel to another part of the testes, where they gain the ability to swim. A duct called the vas deferens transports them and releases them into the ejaculate. “We find very strict control mechanisms at each of those stages,” said Alexander Pastuszak, co-founder of Paterna Biosciences and an adjunct professor at the University of Utah School of Medicine, who is also a urologist. He described the company’s work as the first major innovation in the field since the introduction of intracytoplasmic sperm injection 30 years ago. “We began researching the possibility of growing sperm in vitro and identified the molecular programming of spermatogenesis,” Pastuszak explained in a promotional video last summer. “We used that knowledge to develop an in vitro platform that allows us to grow sperm.” Urologist Larry Lipshultz from Baylor College of Medicine, a specialist in male reproductive health, called the development a major advancement when speaking to WIRED as an external expert. “People don’t understand—or never understood—what growth factors are needed to make these cells mature into sperm. It looks like we’ve identified those substances,” he said. Pastuszak and his team then used the lab-grown sperm to create test embryos, solely to preliminarily validate the safety of the latest method. The embryos appeared healthy, at least temporarily. “It’s a huge leap forward,” Lipshultz added. More than one in eight Americans aged 25 to 49 experience some form of infertility today, according to updated data from the U.S. Department of Health and Human Services. This is a global issue that has driven both public and private research efforts, and progress appears to be underway. The Utah-based biotech, in collaboration with the Mayo Clinic, announced this week that they have successfully cultivated mature, motile sperm in the lab from spermatogonial stem cells. The company says the technique could eventually help men with infertility conceive biological children.
Startup Claims Lab-Grown Sperm Can Produce Embryos, Potentially Revolutionizing Fertility
5