GLP-1 medications like Wegovy and Mounjaro have become increasingly popular for weight loss,offering meaningful results for many who struggle with customary methods. Though, the long-term effects of these drugs remain largely unknown, and discontinuing use presents a unique set of challenges.This report from BBC News examines the experiences of two women, Tanya and Ellen, as they navigate life both on and off these powerful medications, offering a nuanced look at the complex relationship between pharmaceuticals and weight management.
-
- Autor, Ruth Clegg y Holly Jennings
- Título del autor, BBC News
-
Tiempo de lectura: 7 min
“It’s like a switch that flicks and suddenly you’re ravenous.”
Tanya Hall has tried to stop the weight-loss injections several times. But each time, the noise of food returns, and with a vengeance.
Weight-loss injections, or GLP-1 medications, have achieved for many what diets never could: silencing a constant hum that told them to eat even when full.
These medications have given those who never thought they could lose weight a new body shape, a new outlook, and, in many cases, a completely different life. The growing use of these drugs highlights the complex relationship many people have with food and weight management.
But you can’t stay on them forever, can you? Or can you? That’s one of the problems – no one knows for sure.
These are relatively new drugs, which mimic GLP-1, a natural hormone that regulates appetite, and the potential long-term effects of their use are only just beginning to emerge.
In the United Kingdom alone, 1.5 million people are paying for the injections privately, and they aren’t cheap, making continued long-term treatment a significant challenge.
And what happens when you try to stop? Two women, with very different stories but the same goal – to lose weight and keep it off – share their experiences.

Fuente de la imagen, Tanya Hall
“It was like something opened up in my brain and told me, ‘Eat it all, go on, you deserve it because you haven’t eaten anything for a long time.’”
Tanya, a sales manager at a large fitness company, started injecting Wegovy to prove a point. She was overweight, felt like an imposter, and believed her opinions weren’t valued in her work sector because of her size.
Would she be taken more seriously if she were thinner?
Ultimately, she says her suspicions were confirmed. After starting the injections, people approached her to compliment her weight loss. She felt she was treated with more respect.
Over 35 Pounds Lost, But Some Issues
However, during the first few months of treatment, Tanya struggled to sleep, felt unwell constantly, experienced headaches, and even started losing her hair, which may not have been directly caused by the medication, but a possible side effect of rapid weight loss.
“It was coming out in clumps,” she recalls. But in terms of weight, she was getting the results she wanted. She had lost around 16 kilograms (35 pounds).
Now, more than 18 months on, what began as a small experiment has become a total life change. She has lost 38 kilograms (84 pounds) and has tried to come off Wegovy several times.
But each time, within just a few days, she says she eats so much she is “completely horrified.”
Should she continue taking the medication and live with all the side effects, or take the plunge into the unknown?
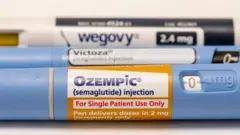
Fuente de la imagen, Getty Images
Novo Nordisk, the manufacturer of Wegovy, stated that treatment decisions should be made in conjunction with a healthcare professional and that “side effects should be considered.”
Stopping weight-loss medication can feel like “jumping into the void,” says Dr. Hussain Al-Zubaidi, a general practitioner specializing in lifestyle medicine.
“I often see patients coming off it when they’re on the highest dose because they’ve reached their goal.”
According to Al-Zubaidi, that can be compared to being hit by an “avalanche or a tsunami.” The noise of food comes back the next day.
He says evidence so far suggests that, one to three years after coming off the medication, people will regain a “significant proportion” of the weight lost.
“Between 60% and 80% of the weight lost will return.”
Compulsive Eater
Ellen Ogley is determined not to let that happen. She decided to start medication to lose weight because she had reached a pivotal point in her life.
She was so overweight she had to sign a waiver saying she might not survive a vital operation.
Starting Mounjaro was her “last chance to get it right,” she says.
“I was an emotional compulsive eater.”
“If I was happy, I’d binge. If I was sad, I’d binge. It didn’t really matter, I had no filter.”
But when she started the medication, “it all just switched off.”

A life without the overwhelming appetite gave Ellen the space to redesign her relationship with food. She began reading about nutrition and creating a healthy diet to fuel her body.
She took the medication for 16 weeks before starting to taper off it, over a period of six weeks. She lost 22 pounds.
As she lost weight, she found she could exercise more, and when she felt down, instead of going to the pantry and filling up, she’d go for a run.
But when Ellen stopped taking Mounjaro, she started to notice weight creeping back on, which, she says, “freaked me out a bit.”
That’s why receiving the right support is crucial, Al-Zubaidi explains.
Practical Changes
The UK’s National Institute for Health and Care Excellence (NICE) has recommended that patients receive at least a year of ongoing support and personalized action plans after coming off treatment, helping them to make practical changes to their lives so they can maintain their weight and, crucially, stay healthy.
But for those paying for the medications privately, like Tanya and Ellen, that kind of support isn’t always guaranteed.
Over the past few months, Tanya has maintained her weight and feels the medication is barely affecting her. But she isn’t going to stop taking it, she says.
She has finally reached a weight where she feels comfortable, and every time she tries to stop, the fear of putting the weight back on becomes too great, and she finds an excuse to start again.
“For the first 38 years of my life, I was overweight; now I’m 38kg lighter,” Tanya says.
“So, part of me feels like there’s an addiction because it makes me feel how I feel, it makes me feel like I’m in control.”
She pauses. Maybe it’s the other way around, she reflects. Maybe the medication is controlling her.

Pie de foto, Ellen has continued to lose weight since coming off weight-loss medication.
“It’s about having an exit strategy,” Al-Zubaidi explains. “The question is, what are people’s experiences once they stop injecting?”
He worries that, without additional support for those transitioning off, society’s unhealthy relationship with food means little will change. The environment people live in needs to be one that promotes health, not weight gain.
“Obesity isn’t a GLP-1 deficiency,” he says.
In a way, many people are entering a kind of weight-loss lottery when they come off their medication. Factors like lifestyle, support, mindset, and timing all influence how the future unfolds after stopping GLP-1.
Tanya continues on the medication and is fully aware of the pros and cons of that decision.
Ellen feels that chapter is closed. She has lost more than 51 kilograms (112 pounds).
“I want people to know that life after Mounjaro can be sustainable too,” she says.
Eli Lilly, the company that manufactures Mounjaro, says that “patient safety is its top priority” and that it “actively engages” in monitoring, evaluating, and submitting information to regulatory bodies and physicians.

Suscríbete aquí to our new newsletter to receive a selection of our best content each Friday.
And remember you can receive notifications in our app. Download the latest version and activate them.
